Benign and malignant lesions of the cervix

Benign and malignant lesions of the cervix

Benign and malignant lesions of the cervix
Identifying the premalignant and benign diseases of the cervix and choosing an appropriate treatment is often a challenge for the specialist, because the adult cervix can present a wide variety of pathological diseases. These conditions may be benign (e.g., inflammation of the cervix called cervicitis, Nabothian cysts, cervical polyps, myomas, endometriosis, and congenital abnormalities), as well as malignant lesions, especially cervical carcinoma.
Cervical lesions vary by size, from being visible by colposcopy (the small ones) to being visible by speculum examination or by transvaginal ultrasound (the larger ones).
The most common types of benign entities present in the cervix are:

1. Cervical polyps
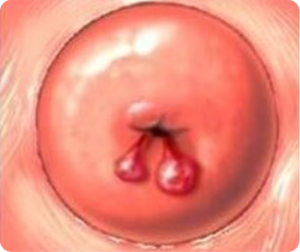
Are the most common benign formation found in the cervix. They are small in size and occur mainly in women over 20 years of age. They may be the consequence of pregnancy, an excess of oestrogen hormones, or they may be the result of chronic infections and inflammations.
Cervical polyps can vary in size, shape, and origin. They can present themselves as a single entity or as a group of polyps, they have different shapes, they are reddish cherry or white-gray, depending on the vascularity of the lesion. The size of the cervical polyp is usually less than three cm in diameter. However, they can vary in size and be large enough to fill the vagina. In some cases, they can become infected and lead to vaginal discharge. In other cases, they can block menstrual flow. In severe cases, it can lead to infertility, by blocking the cervix and obstructing the lining of the uterus. Removal of polyps is necessary because they can become infected and can become cancerous.
2. Naboth's cysts
Are a type of lump, of small size (from a few mm to 4 cm), filled with liquid content, which often occurs at the age of reproduction. They have no clinical significance. These cysts form in the cervix, when the own cells in the outer area of the cervix (also called the ectocervix) grow in the region of the cervix opening to the uterus (the area called endocervix). As a result of this growth, the ducts of the mucus-producing glands become obstructed, and the mucus accumulates in them. Cysts contain mucus, but may also contain proteinaceous materials, neutrophils, or neutrophil debris. These cysts usually appear superficial and are easily recognizable during colposcopy. They can also be formed after a cervical injury. In the absence of treatment, Naboth’s cysts can induce considerable cervical enlargement. Nabothian cysts can be surgically removed, can be cauterized, or treated with cryotherapy (with liquid nitrogen cooled at very low temperatures).

3. Genital warts
Genital warts (also called acuminate warts) are small, cluster-like tumour lesions that occur in the cervix following HPV infection. Condylomas tend to form plaques. They can promote microbial or fungal infections and can evolve into cervical cancer. Genital warts cause itching, dysuria, discomfort, and leucorrhoea. They can be treated by cryotherapy, electrocautery, laser therapy or curettage.

4. Cervical fibroids
Cervical fibroids (myomas) begin to develop in the muscle tissue of the cervix. They’re consistent with uterine fibroids, but less frequent. Cervical fibroids generally do not produce symptoms. Sometimes they can cause abnormal vaginal bleeding or pain during or after intercourse. If the fibroid enlarges, it can partially block the urinary tract and cause problems, such as urinary retention. If myomas become infected, they may cause pain, bleeding, or leucorrhoea. The recommended treatment in all cases is excision. After surgery, it is very important to apply a local haemostatic and reepithelialising treatment for a rapid recovery.
Following the surgical intervention, the specialist doctor may prescribe Cerviron® ovules with a repairing and anti-inflammatory effect. Through bismuth subgallate with haemostatic effect, Cerviron® ovules support a rapid recovery and promote the restoration of the specific vaginal flora.
Read more about the benefits of using Cerviron® for post operatory care.












